Does Ambetter Cover Ozempic for Weight Loss?
Ambetter generally does not cover Ozempic when it’s prescribed just for weight loss. Ozempic (semaglutide) is an FDA-approved diabetes drug, not an obesity drug. Ambetter’s policy follows this distinction: their drug lists show Ozempic covered only for Type 2 diabetes. In fact, Ambetter explicitly states that GLP-1 drugs “are not currently covered when prescribed solely for weight management”. In practice this means if your doctor writes Ozempic for weight loss (an off-label use), Ambetter will likely deny it, and you’d have to pay the full cost.
Ozempic vs. Wegovy: What Ambetter Lists
Ozempic and Wegovy are actually the same medication (semaglutide) in different doses. Ozempic is FDA-approved for diabetes; Wegovy is FDA-approved for chronic weight management. Ambetter’s plan formulary makes the coverage difference clear. For example, in one Ambetter plan Ozempic (for Type 2 diabetes) is listed as a covered drug (though non-preferred/high tier). By contrast, Wegovy (for obesity) is explicitly a non-covered benefit. Similarly, Ambetter guidance notes that weight-loss GLP-1 prescriptions are non-covered. In other words, Ambetter will pay for Ozempic only if you use it to manage diabetes. If your goal is weight loss, Ambetter treats Ozempic as out-of-pocket, and even the approved weight-loss version (Wegovy) is typically excluded.
Why Ozempic Isn’t Covered for Weight Loss
Ambetter’s stance comes down to FDA approvals and medical necessity. Ozempic is labeled for blood sugar control in diabetes, not for dieting or obesity. Using it for weight loss is considered “off-label.” Most insurance companies, Ambetter included, refuse to cover off-label uses unless there’s a compelling reason. Ambetter’s official materials make this clear: GLP-1 drugs (like Ozempic) “are not covered when prescribed solely for weight management”. In short, if your Ambetter plan sees Ozempic used only for losing weight, they’ll deny coverage. Only when Ozempic is prescribed to treat a covered condition (Type 2 diabetes with medical justification) will Ambetter consider paying for it.
Prior Authorization and Formularies
Even when Ozempic is covered (for diabetes), Ambetter typically requires prior authorization. This means your doctor must document that Ozempic is medically necessary under the plan’s rules. Ambetter’s drug tiers also impact costs: in many state plans Ozempic sits in a higher tier (“Non-Preferred” or “Specialty”). You may have to try cheaper diabetes drugs (like metformin) first before Ambetter approves Ozempic. On the other hand, weight-loss drugs like Wegovy or Saxenda (liraglutide for obesity) are often entirely excluded. For example, Ambetter’s formulary notes Wegovy as a non-covered benefit. This underscores that Ambetter will not pay for Ozempic simply to help you shed pounds.
What This Means for You
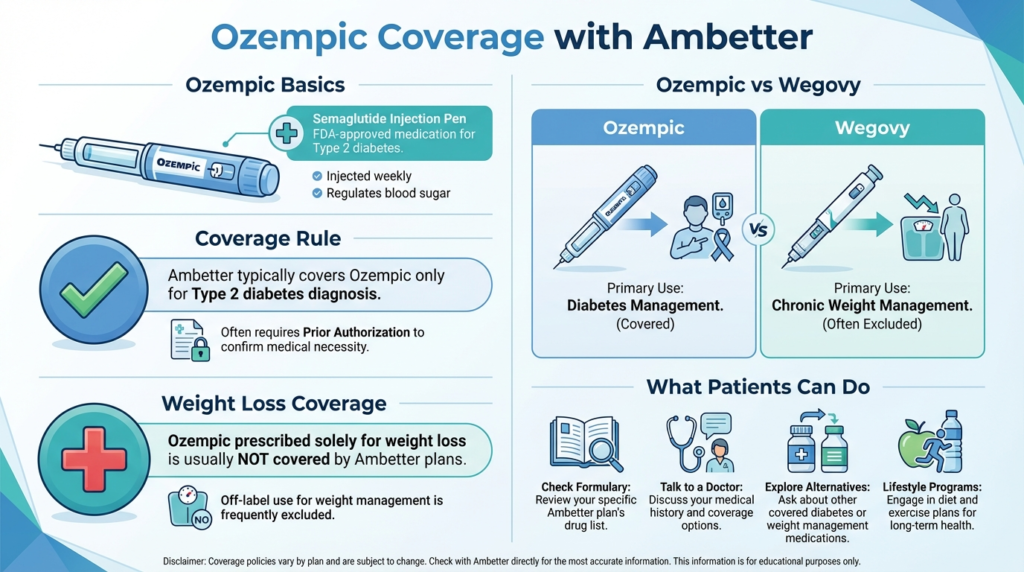
If you have Type 2 diabetes and your doctor prescribes Ozempic, Ambetter can cover it – but only after prior authorization and proof of medical need. However, if you don’t have diabetes and want Ozempic to lose weight, be prepared to pay out of pocket. Ozempic’s list price is high (often over $1,000 per month), so Ambetter’s denial could mean a large expense on your part. Before deciding how to proceed, consider these steps:
- Check Your Plan’s Drug List. Look up your Ambetter plan’s formulary (online or in your member portal) to see how Ozempic and weight-loss drugs are listed. Note if Ozempic requires prior authorization or step therapy. Confirm whether Wegovy or other GLP-1 weight-loss drugs are covered (often they’re not).
- Talk to Your Doctor. Explain Ambetter’s rules: Ozempic is covered only for diabetes. If you have diabetes (or pre-diabetes) and qualify, your doctor can submit the paperwork (prior authorization) to Ambetter to get Ozempic approved. If your only issue is weight, ask about FDA-approved obesity drugs instead.
- Explore Alternatives. FDA-approved weight loss medications include Wegovy (semaglutide) and Saxenda (liraglutide). Although Ambetter often excludes these, it’s worth asking your doctor if any covered alternatives exist (like older weight-loss drugs) or if any weight management programs are offered by Ambetter.
- Plan for Costs if Needed. If Ambetter denies Ozempic for weight loss, you’ll be responsible for the full price. You might look into manufacturer savings cards or patient assistance programs (Novo Nordisk offers Ozempic/Wegovy copay cards for eligible patients). Using a flexible spending account (FSA) or health savings account (HSA) for these costs can also help.
- Lifestyle Support. Regardless of medications, Ambetter often covers lifestyle programs. Take advantage of nutrition counseling, exercise programs or health coaching through Ambetter to support your weight goals within what the plan covers.
Ambetter’s official line is consistent: GLP-1 drugs are for diabetes treatment, not a weight loss benefit. In practice, this means Ozempic won’t be covered for weight loss. Always verify with your specific Ambetter plan (and state) by reviewing the drug coverage section or calling customer service. Your doctor and Ambetter customer service can clarify your options so you can make an informed choice. The bottom line is: Ambetter covers Ozempic only as a diabetes drug, and you’ll need that diagnosis on record for any coverage.